Elizabeth Hofheinz, M.P.H., M.Ed.
Citing a need for more rigorous research as to the real utility of arthroplasty in treating complex proximal humerus fractures, a group of scientists from multiple institutions got to work. Their study, “Are Arthroplasty Procedures Really Better in the Treatment of Complex Proximal Humerus Fractures? A Comprehensive Meta-Analysis and Systematic Review,” appears in the March 2021 edition of the Journal of Orthopaedic Trauma.
Co-author Richard Yoon, M.D., an orthopedic surgeon at Jersey City Medical Center—RWJ Barnabas Health, told OSN: “Arthroplasty (specifically reverse shoulder arthroplasty) continues to gain traction as an acceptable treatment for proximal humerus fractures in the elderly. Other studies comparing the two have shown mixed results (superiority or inferiority) but they tried to compare studies that were not truly comparable. We aimed to produce a meta-analysis that exhibited the holes in the current literature and wanted to express a need for higher level trials to definitively determine which procedure is superior.”
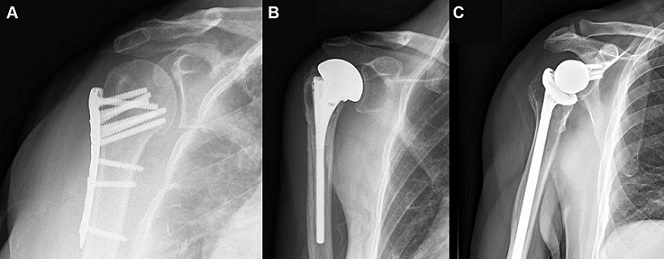
The researchers looked at studies published (in English) within the last 15 years that assessed the outcomes of open reduction and internal fixation (ORIF), reverse total shoulder arthroplasty (rTSA), or hemiarthroplasty (HA) for complex proximal humerus fractures. They ended up with 51 with 3,064 total patients. While randomized controlled trials, prospective or retrospective cohort studies, and case series were included, review articles, basic science studies, biomechanical studies, and cadaveric studies were excluded.
The most commonly reported outcome measures were Disabilities of the Arm, Shoulder, and Hand (DASH) and Constant scores.
The authors wrote, “Patients undergoing rTSA had lower risks of complication and reoperation than HA patients. rTSA resulted in higher Constant scores and improved active forward flexion when compared to HA. Pooled mean data demonstrated better outcome scores and active forward flexion of ORIF versus HA and rTSA, though the patients were younger and had more simple fracture patterns…DASH scores were slightly lower in patients undergoing rTSA versus HA.” The authors note that DASH is a disability measure, and thus lower scores represent better outcomes.
“We found that it was extremely difficult to do a true head-to-head comparison with the available literature,” stated Dr. Yoon to OSN. “Reverse arthroplasty exhibited superior outcomes in some areas (lower revision rate), while ORIF exhibited higher functional outcomes in some comparisons. All were better than hemiarthroplasty (which we no longer do or should do in the elderly).”
If there is a next step, says Dr. Yoon, it will be a level 1 randomized control trial comparing reverse to ORIF.
As for what he would like his colleagues to know, Dr. Yoon told OSN, “Do what you’re good at! The jury is still out—but the data (and personal experience) seems to lean towards both surgeon experience/comfort level along with severity of the fracture pattern. In the elderly, the more comminuted the fracture, and for those with a dislocation, a reverse is probably the way to go. For operative fractures not as severe, ORIF may still be the treatment of choice.”