Elizabeth Hofheinz, M.P.H., M.Ed.
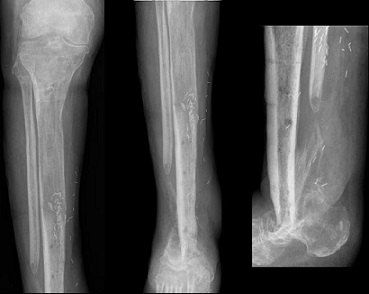
In looking at 211 nonunions (204 patients), researchers from several institutions have determined that commonly gathered biomarker information may not be so helpful in predicting infection. Their work, “Utility of Common Biomarkers for Diagnosing Infection in Nonunion,” appears in the March 2021 edition of the Journal of Orthopaedic Trauma.
Co-author Warren R. Dunn M.D., M.P.H. is with the Fondren Orthopedic Research Institute in Houston, Texas. Dr. Dunn told OSN, “Dr. Mark Brinker’s practice sees a high volume of nonunions and his observation was that these biomarkers did not seem to correlate well with septic nonunion.”
The authors considered leukocyte count (WBC), erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP) in order to determine whether a nonunion was septic or aseptic.
The authors note, “Inclusion criteria were consecutive patients (≥18 years) with a nonunion requiring surgery that allowed for direct or medullary canal tissue sampling from the nonunion site…”
Preoperative blood samples were drawn to determine WBC, ESR, and CRP.
“The reference standard used to define infection was the fracture-related infection confirmatory criteria,” wrote the authors. “Measures of diagnostic accuracy were calculated. To assess the additional diagnostic gain of each index lab test while simultaneously considering the others, logistic regression models were fit.”
Dr. Dunn commented to OSN: “In a consecutive series of all nonunions with a spectrum of clinical presentation where the diagnosis of infection is unclear, these biomarkers were not predictive of septic nonunion.”
Specifically, wrote the authors, “The prevalence of infection was 19% (40 of 211 nonunion sites). The positive likelihood ratios (95% confidence interval) for WBC, ESR, and CRP were 1.07 (0.38-3.02), 1.27 (0.88-1.82) and 1.57 (0.94-2.60), respectively. Multivariable modeling adjusted for the effect of preoperative antibiotics showed that WBC (P = 0.42), ESR (P = 0.48), and CRP (P = 0.23) were not significant predictors of infection.”
“I think it would be useful,” said Dr. Dunn to OSN, “to know how often patients are treated for septic nonunion based, at least in part, on the results of these biomarkers when in fact they have an aseptic nonunion and what is the burden of that treatment to the patient. Such as the cost, side effects, etc. of prolonged antibiotic treatment that is potentially unnecessary.”
“Standard clinical practice is to obtain these biomarkers on all nonunions to rule out infection, however, these biomarkers really do not have much utility in this regard and more emphasis might be placed on other clinical data as well as the clinician’s gestalt.”
Note: Dr. Brinker is affiliated with the Fondren Orthopedic Research Institute, Fondren Orthopedic Group, and Texas Orthopedic Hospital.