Elizabeth Hofheinz, M.P.H., M.Ed.
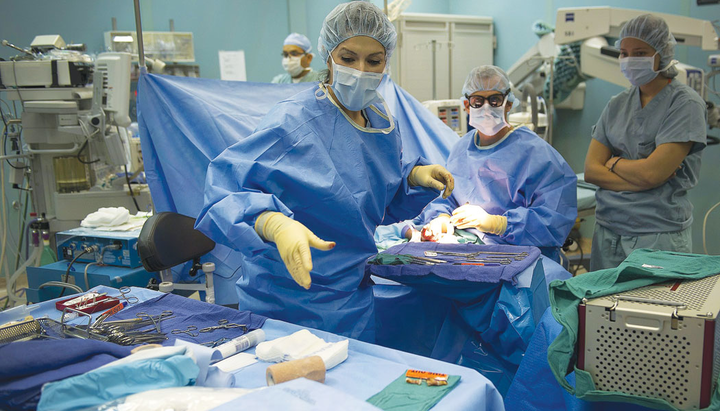
A new retrospective review including data on 11,163 patients has found that the size of the OR makes a significant difference in the development of a surgical site infection (SSI).
The multicenter work, “The Effect of Operating Room Size on Orthopaedic Surgical Site Infection Rates,” appears in the January 13, 2021 edition of The Journal of the American Academy of Orthopaedic Surgeons.
“In relatively smaller ORs,” write the authors, “the distance between sterile and nonsterile fields—defined as the ‘margin of safety’ (a minimum of 12 inches)—is shorter than that of relatively larger ORs. Because infection risk increases with any breaks in the sterile field and the available working space is reduced in a smaller OR, the infection risk is expected to be greater in smaller ORs, where the personnel-to-NSF [net square feet] ratio is higher. Consequently, we hypothesize that OR size is inversely related to orthopaedic SSIs—a decrease in NSF corresponds to an increase in the SSI rate.”
Co-author Tyler J. Tantillo, D.O. is with the Department of Orthopedic Surgery at the Donald & Barbara Zucker School of Medicine at Hofstra/Northwell, Plainview Hospital, Plainview, New York. Dr. Tantillo commented to OSN, “The main reason for conducting this study was that we noticed that there was a lot of variability among the sizes of operating rooms within our health system. Ultimately, we wanted to better understand if the size of the operating room had any effect on the development of am SSI, and if so, what was the relationship.”
“At the time, to our knowledge, other factors such as operating room personnel and airflow had been examined with respect to the development of an SSI, however, no studies specifically investigated the size of the operating room. If a relationship existed between operating room size and the development of a SSI, then the future construction of operating rooms could be modified to improve patient outcomes, which was the goal of our study.”
The study, which comprised five community hospitals and three tertiary care centers, looked at the following procedures: total knee arthroplasty (TKA), total hip arthroplasty (THA), laminectomy, and spinal fusion. The team had infection preventionists review all laboratory data, postsurgical readmissions, and returns to the OR. The net square feet were calculated for all 78 ORs; each OR had a vertical unidirectional linear airflow diffuser system, with positive pressure ventilation and a minimum of 20 air exchanges per hour (at least 4 were outside air). Temperature and humidity in the ORs were kept between 68 ° to 75 °F and 30% to 60%, respectively.
“Our study showed that medium-sized operating rooms (400-549 net square feet) had a statistically significant association with the development of an orthopedic surgical site infection,” stated Dr. Tantillo. “Akin to other previously published studies, we also found that younger patients, procedure type (spinal fusions and emergencies/traumas), longer procedures, and higher American Society of Anesthesiologists scores (>3) were statistically associated with increased SSI rates.”
“The next steps of this study entail conducting a double-blinded prospective trial whereby patients with matched demographics undergoing the same procedure would be randomized to operating rooms with varying sizes. Ideally, confounding variables such as preoperative antibiotics, number of operating room personnel, airflow systems etc. would be consistent among procedures. Post-operatively, patients would be followed for at least 90 days to observe for the development of a surgical site infection.”
Looking forward, Dr. Tantillo told OSN: “We hope that our study continues to generate discussion on how we can optimize the surgical environment to improve patient outcomes. We look forward to continuing our research in the near future with the aim to reduce orthopedic surgical site infections and to advance the field of orthopedic surgery.”